Thyroid cancer is one of the most common cancers of the endocrine system, with increasing diagnoses in both men and women globally, including in India. While thyroid cancer is relatively rare compared to other cancers, its incidence has been steadily rising, especially in urban areas. The good news is that thyroid cancer, when diagnosed early, is highly treatable with excellent survival rates.
Dr. Sandeep Nayak, a well-known surgical oncologist in India, states, “With early detection and appropriate treatment, most patients with thyroid cancer can expect a full recovery, making regular screenings and timely intervention essential.” However, the question of whether thyroid cancer can be fully cured depends on its type, stage, and the patient’s overall health.
With extensive expertise in thyroid procedures, Dr. Nayak is dedicated to guiding patients through every stage of their treatment, maximizing their chances of long-term health and recovery. He offers comprehensive thyroid cancer treatment in Bangalore, with a focus on the latest modalities and personalized care.
Having years of experience in treating complex thyroid conditions, Dr. Nayak’s approach combines advanced, minimally invasive surgical techniques with effective follow-up strategies. He ensures that every patient receives the highest level of care tailored to their individual needs.
What is Thyroid Cancer?
Thyroid cancer develops when cells in the thyroid gland grow uncontrollably. The thyroid, located in the neck, produces hormones that regulate metabolism, body temperature, and heart rate.
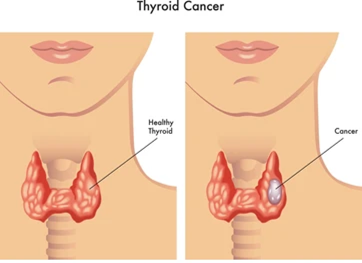
When cancerous cells form, they can either be localized or spread to other parts of the body. Thyroid cancer is typically identified when a lump or nodule is found in the neck, often through routine exams or imaging tests.
How do different types of thyroid cancer affect the chance of a cure? Let’s look at the types.
Types of Thyroid Cancer and Their Cure Rates
There are four main types of thyroid cancer, and their cure rates vary:
- Papillary Thyroid Cancer (PTC):
The most common form, making up about 80% of cases. It has an excellent prognosis with a high cure rate (over 90% if caught early).
- Follicular Thyroid Cancer (FTC):
Less common but still treatable. It also has a good prognosis with cure rates of around 80-90%.
- Medullary Thyroid Cancer (MTC):
A rarer type that may have a more challenging treatment course, but with early detection, the cure rate is around 70%.
- Anaplastic Thyroid Cancer (ATC):
The most aggressive form, which is difficult to treat and has a lower cure rate, often under 10%.
Wondering about the available treatment options? Let’s dive into it
Treatment Options for Thyroid Cancer
Thyroid cancer treatment depends on the type and stage of cancer, as well as the patient’s overall health. The treatment methods are:
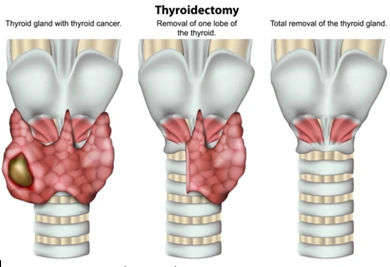
This is the most common treatment method, which entails the removal of affected tissue or the entire thyroid gland.
* Radioactive Iodine Therapy
After surgery, this treatment may be used to destroy any remaining cancer cells.
* External Radiation Therapy
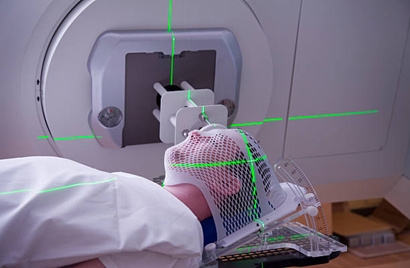
Radiation treatment is applied in specific cases where it targets and shrinks the tumor, especially when dealing with anaplastic cancer.
* Targeted Therapy
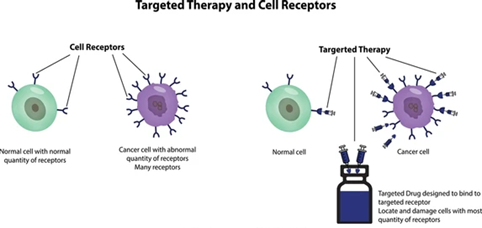
In cases of medullary thyroid cancer or advanced disease, targeted drugs can help inhibit cancer cell growth.
Factors That Affect Survival Rates
o Cancer type: Papillary and follicular thyroid cancer typically have a higher survival rate than medullary or anaplastic types.
o Stage at diagnosis: Early-stage cancer is easier to treat, hence it offers better chances of success.
o Age: Younger individuals generally have better outcomes.
o Overall health: A person’s general health status impacts recovery from cancer.
How long can patients live with thyroid cancer? Let’s find out
What Is the Survival Rate of Thyroid Cancer?
Survival rate for thyroid cancer largely depends on the type, stage, and the patient’s overall health. For papillary and follicular thyroid cancer, the 5-year survival rate is typically above 90%, especially when detected early and treated effectively.
Medullary thyroid cancer has a somewhat lower survival rate. It ranges from 70-80% as this type tends to be more aggressive and harder to treat. Anaplastic thyroid cancer, the rarest and most aggressive, has a much lower survival rate, often under 10%, since it spreads rapidly and is difficult to manage.
Can Thyroid Cancer Come Back?
Yes, thyroid cancer can come back. Likelihood depends on various factors, such as the type of thyroid cancer, stage at diagnosis, and effectiveness of initial treatment. Papillary and follicular thyroid cancer have a relatively low recurrence rate, especially when treated early. Medullary and anaplastic may have a higher chance of recurrence.
“Recurrence can occur locally, within the thyroid bed, or even at distant sites like the lungs or bones. This is why regular follow-up care is crucial,” states Dr. Sandeep Nayak, an esteemed surgical oncologist in Bangalore. Imaging tests, blood tests to check thyroid hormone levels, and ultrasounds are commonly used to monitor for any signs of recurrence.
How can you maximize your chances of recovery? Here are some tips
Tips to Improve Outcomes and Recovery
- Follow your doctor’s instructions regarding post-treatment care, including medication and lifestyle changes.

- Maintain a healthy diet to support your recovery and overall well-being.
- Attend regular follow-up appointments to monitor your thyroid function and ensure cancer does not return.

- Stay active with appropriate exercise, as recommended by your doctor, to enhance recovery and prevent complications.
Frequently Asked Questions
1. When Is Surgery Recommended for Thyroid Cancer?
2. Can Thyroid Cancer Be Cured?
3. Can Thyroid Cancer Return?
4. What Are the Side Effects of Thyroid Cancer Treatment?
5. What Is the Recovery Time After Thyroid Cancer Surgery?
Reference links:
https://www.mayoclinic.org/diseases-conditions/thyroid-cancer/diagnosis-treatment/drc-20354167
https://www.mayoclinic.org/diseases-conditions/thyroid-cancer/diagnosis-treatment/drc-20354167
Disclaimer: The information shared in this content is for educational purposes and not for promotional use.


