


Bengaluru surgeon among top 3 winners in International Robotic Surgery

Chemotherapy for Rectal Cancer
Rectal cancer is a growing concern globally and in India, often requiring a combination of therapies for effective treatment. According to the World Health Organization (WHO), colorectal cancer (which includes rectal cancer) is the third most common cancer worldwide, with over 1.9 million cases reported in 2022. India is witnessing a steady rise in these numbers, particularly in urban populations, due to changing lifestyles, dietary habits, and late detection. This makes timely treatment even more essential.
According to Dr. Sandeep Nayak, an experienced surgical oncologist in Bangalore:
“Chemotherapy plays a vital role in managing rectal cancer. In essence, it supports every phase of the treatment—from preparation and precision in surgery to long-term protection after recovery. For patients who aren’t fit for surgery or prefer a non-operative approach, chemotherapy takes a leading role in managing the disease.”
This page will guide you through when and why chemotherapy is used, what to expect during treatment, how to manage side effects, and what life looks like after treatment.
Let’s begin with the basics.
When Is Chemotherapy Used in Rectal Cancer?
Chemotherapy isn’t used for every rectal cancer patient. Its role depends on the cancer’s stage, location, and whether it has spread.
Here’s when chemotherapy becomes essential:
Before surgery (neoadjuvant chemotherapy): To shrink the tumor, making it easier to remove surgically.
After surgery (adjuvant chemotherapy): To kill any remaining cancer cells and reduce the risk of recurrence.
In advanced stages: If the cancer has spread to distant organs (metastatic rectal cancer), chemotherapy becomes a key player in symptom management and prolonging life.
In India, many patients are still diagnosed in Stage III or IV due to lack of routine screening, making chemotherapy a crucial intervention in most cases.
How Chemotherapy Helps in Rectal Cancer Treatment
Chemotherapy contributes significantly at different stages of care. Here’s how it works:
Tumor Shrinkage Before Surgery
Many patients present with large tumors that cannot be safely removed in one go. Chemotherapy helps shrink the tumor to a size that makes surgical removal easier and reduces the risk of leaving behind cancerous tissue.
Targeting Cancer Cells
Cancer cells may spread to other organs even if they aren’t visible on scans. Chemotherapy targets and destroys these microscopic cancer cells—whether they’re detected or not—before surgery, helping to clear the body of cancer.
Enhancing the Effect of Radiation (Radiosensitization)
Chemotherapy increases the sensitivity of cancer cells to radiation, allowing for better tumor control and improved results from radiotherapy.
Post-Surgical Cleanup of Remaining Cancer Cells
After surgery, some cancer cells may still linger undetected. Chemotherapy helps eliminate these residual cells, which cannot be picked up by scans or tests, thereby reducing the chances of recurrence and improving overall survival.
Identifying symptoms early can help control LARS better. Speak with a specialist for a personalized evaluation.
What to Expect During Chemotherapy
Chemotherapy for rectal cancer usually involves a combination of drugs administered in cycles, either through intravenous infusion or oral tablets. Each cycle is followed by a rest period to allow your body to recover. The total duration typically ranges between 6 to 8 months, depending on the individual’s case and response to treatment.
During your treatment sessions:
- You’ll spend a few hours at a clinic or hospital.
- Blood tests may be done before each cycle.
- You’ll be monitored for any immediate side effects.
- Medications will be prescribed to manage nausea, fatigue, and other issues.
The experience is different for everyone, and most patients are able to go home the same day.
Common Side Effects and How to Manage Them
Here are the most common side effects and tips to cope with them:
| Side Effect | Management Tips |
|---|---|
| Fatigue | Prioritize rest, stay hydrated, and keep light physical activity in your routine. |
| Nausea/Vomiting | Anti-nausea medications help; eat small, bland meals frequently. |
| Diarrhoea | Stay hydrated, avoid spicy foods, and inform your doctor for medication. |
| Neuropathy | Common with Oxaliplatin. Report tingling or numbness to your care team. |
| Hair thinning | Less common than in other cancers, but possible. Consider head coverings for comfort. |
Proactive communication with your oncologist and care team ensures timely adjustments and improved quality of life during therapy.
Yes—and mostly in a good way.
Impact of Chemotherapy on Surgery and Recovery
Post-surgery, chemotherapy may delay wound healing slightly, but this is usually temporary and well-managed by your medical team.
Dr. Nayak a trusted surgical oncologist in India, shares:
“Every patient deserves a personalized treatment approach that takes their specific cancer stage and health into account. When patients undergo chemotherapy before surgery, we often see improved surgical outcomes and better long-term results. The key is careful planning between surgical and medical oncologists to time everything just right.”
Life After Chemotherapy: Recovery & Long-Term Care
The journey doesn’t stop with the last infusion. Post-chemotherapy life involves regular follow-ups, scans, and lifestyle adjustments to monitor your health and prevent recurrence. Recovery is a team effort—and timing, nutrition, and close monitoring all play their part.
Here’s what long-term care includes:
- Routine scans (CT, MRI, colonoscopy) every 6 to 12 months initially.
- Blood tests, especially for tumor markers like CEA.
- Nutritional counselling to rebuild strength and support digestion.
- Psychosocial support to manage anxiety and regain normalcy.
Many patients in India worry about returning to work, diet restrictions, or sexual health after chemo. With good support, most return to normal or near-normal life within months.
Conclusion
Chemotherapy for rectal cancer is a powerful tool in the modern cancer care toolkit. It helps improve survival, shrink tumours, and reduce the chance of cancer coming back. While it’s not without challenges, the benefits often far outweigh the discomfort—especially when guided by an experienced oncology team.
Whether you’re preparing for surgery, recovering, or managing advanced disease, chemotherapy may play an essential role in your treatment plan.
Frequently Asked Questions
Is chemotherapy required for all rectal cancers?
Not always. Its necessity depends on the cancer’s stage, size, and spread. Early-stage rectal cancers might only need surgery, while more advanced cases typically benefit from chemotherapy.
How long does chemotherapy for rectal cancer last?
Chemotherapy usually lasts 6 to 8 months, delivered in cycles with rest periods in between. The duration can vary depending on how well your body responds to the treatment.
Can chemotherapy alone cure rectal cancer?
Chemotherapy alone is not curative for rectal cancer. It’s most effective when combined with surgery and/or radiation, depending on the cancer stage.
What foods should I avoid during chemo?
Avoid raw or undercooked foods, spicy meals, and high-fat items that can upset your stomach. Eat well-cooked, balanced meals and stay hydrated.
Does chemo affect bowel movements permanently?
Bowel habits may change temporarily during treatment. Most patients see improvement within months, though some may experience longer-term changes depending on surgery or radiation.
Can I work while undergoing chemotherapy?
Yes, many people continue working during chemotherapy, though adjustments may be needed based on fatigue or side effects. Flexibility in your schedule helps manage energy levels.
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.
Neoadjuvant Therapy in Rectal Cancer
Rectal cancer is among the leading causes of cancer-related illness across the world. Globally, colorectal cancer ranks third in terms of incidence and second in terms of cancer-related deaths. In India, rectal cancer is increasingly being diagnosed at more advanced stages due to low awareness and lack of regular screening—especially in rural and semi-urban populations.
That’s where neoadjuvant therapy plays a crucial role. This pre-surgical treatment approach improves surgical outcomes and, in some cases, may help avoid surgery altogether.
Dr. Sandeep Nayak, a seasoned Surgical Oncologist in India, explains:
“Neoadjuvant therapy allows us to gain the upper hand before surgery begins. By shrinking the tumor and targeting unseen cancer cells, we create better conditions for long-term success. It’s a forward-thinking strategy that is now considered standard in managing advanced rectal cancer.”
This guide explains what neoadjuvant therapy is, why it’s used, and how it’s transforming rectal cancer treatment in India and around the globe.
Why Is Neoadjuvant Therapy Used in Rectal Cancer?
Neoadjuvant therapy refers to treatments given before surgery. These can include:

Chemotherapy: A combination of chemotherapy and radiotherapy (chemoradiation)
Immunotherapy: In certain trials or advanced cases
Regardless of the specific therapy, if it’s administered before surgery, it is termed neoadjuvant therapy.
But why treat cancer before surgery at all?
The answer lies in strategy. When cancer is first detected, especially in the rectum, it may already be large or close to vital structures. Jumping straight to surgery without first controlling the disease could result in less effective outcomes or unnecessary complications.
Neoadjuvant therapy helps doctors shrink the tumor, assess how it responds to treatment, and better plan the surgical procedure for safer, more precise removal.
Still wondering why it matters? Let’s dig deeper.
Benefits of Neoadjuvant Therapy in Rectal Cancer
Tumor Downstaging
The primary benefit is shrinking the tumor. By making the tumor smaller before surgery, it becomes easier to remove while preserving healthy tissue.
Improved Surgical Margins
Surgery is all about precision. Neoadjuvant therapy helps clear the tissue planes around the tumor. This means that when the surgeon operates, there’s a higher chance of completely removing the cancer with “clear margins”—areas free of cancer cells.
Lower Recurrence Rates
By targeting cancer cells early, neoadjuvant therapy reduces the risk of local recurrence. This improves the long-term success rate and overall survival.
Organ Preservation (In Select Cases)
One of the most exciting advances in recent years is the potential to avoid surgery altogether in select patients. Those who have an exceptional response to neoadjuvant therapy may be managed with a “wait-and-watch” approach, sparing them the side effects and complications of rectal surgery. While this isn’t suitable for everyone, it’s a life-changing option for those who qualify.
Dr. Sandeep Nayak, an eminent Surgical Oncologist in Bangalore, shares:
“Organ preservation is a major leap forward in rectal cancer care. In select cases, avoiding surgery is not only safe but also significantly improves quality of life. But careful selection and follow-up are key to making this work effectively.”
Now, let’s explore the types of neoadjuvant therapy commonly used.
Types of Neoadjuvant Therapy in Rectal Cancer
Neoadjuvant Chemoradiation
This is the most commonly used form. Chemotherapy drugs are given alongside radiation therapy to shrink the tumor and increase the effectiveness of both treatments.
Neoadjuvant Chemotherapy Alone
In certain cases, especially when radiation isn’t appropriate, chemotherapy alone may be used. This approach is being studied more frequently, particularly in cases with distant metastases.
Short-Course Radiotherapy (SCRT)
A quicker form of radiation therapy often completed in a week, SCRT is sometimes followed by delayed surgery and is particularly useful for patients who can’t tolerate longer radiation courses.
Total Neoadjuvant Therapy (TNT)
A newer and increasingly popular approach where all chemotherapy and radiation are completed before surgery. TNT improves tumor response and reduces the risk of systemic spread.
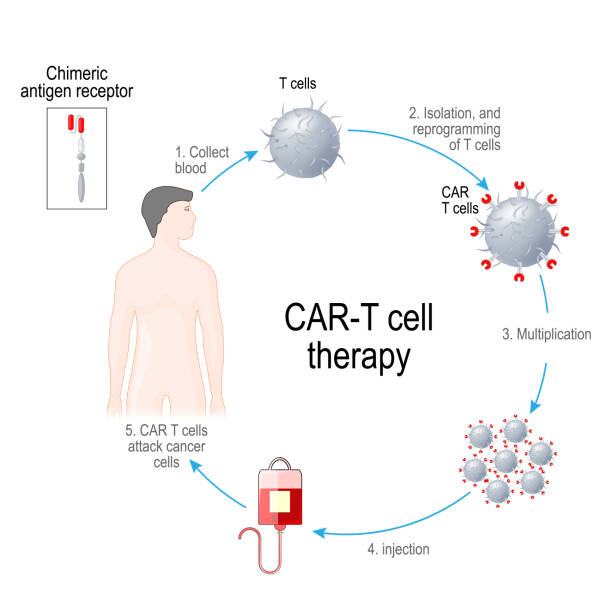
Immunotherapy (in selected cases)
Although not yet standard, ongoing trials are exploring the use of immune-based therapies in rectal cancers, particularly for patients with a specific genetic condition known as mismatch repair deficiency (dMMR).
Dr. Sandeep Nayak explains:
“Mismatch repair deficiency, or dMMR, is a genetic alteration where the body’s natural ability to repair DNA damage is impaired. In such cases, tumors are more likely to respond to immunotherapy because they produce more mutations, making them easier for the immune system to recognize and attack. Identifying this condition early opens doors to highly effective, targeted treatment options.”
Treatment Protocol: What to Expect
Here’s what you can typically expect if you’re prescribed neoadjuvant therapy:
Step 1: Diagnostic Work-up
This includes scans (MRI, CT, PET), colonoscopy, biopsy, and tumor marker tests to determine the exact stage and plan the treatment.
Step 2: Therapy Begins
Most patients receive therapy for 5–6 weeks. If chemoradiation is planned, it’s usually done five days a week over five weeks, with chemotherapy taken orally or intravenously.
Step 3: Waiting Period
After treatment ends, patients wait for about 6–8 weeks to allow the tumor to shrink further and recover from therapy side effects.
Step 4: Assessment
Another scan or evaluation is performed to assess tumor response. Based on the results, patients either proceed to surgery or, in rare cases, are considered for non-surgical monitoring.
Now let’s talk results.
Effectiveness and Clinical Outcomes

Neoadjuvant therapy has revolutionized rectal cancer care. Here’s how:
Increased tumor resectability: Tumors that were once considered inoperable can now be safely removed after therapy.
Better survival rates: Numerous studies, including data from Indian institutions, show improved 5-year survival rates in patients who receive neoadjuvant therapy.
Lower local recurrence: Especially when combined with precise surgical techniques, this therapy reduces the chance of the cancer returning to the pelvis.
Organ preservation rates: In some studies, up to 20% of carefully selected patients avoided surgery altogether.
Indian oncology centers, especially those in urban hubs like Bangalore, are increasingly offering advanced neoadjuvant protocols with outcomes comparable to global standards.
Conclusion
Neoadjuvant therapy in rectal cancer is not just a pre-surgical formality—it’s a transformative approach that enhances surgery, lowers recurrence, and in some cases, replaces surgery altogether. With proper staging, planning, and execution, it leads to better outcomes and, importantly, more tailored, patient-friendly treatment plans.
If you or a loved one is navigating a rectal cancer diagnosis, discussing the possibility of neoadjuvant therapy with an expert may open up better, more effective treatment pathways.
FAQs
Is neoadjuvant therapy necessary for all rectal cancer patients?
No, not every patient requires it. It is typically recommended for those with stage II or III tumors, where it can improve outcomes significantly.
How long does neoadjuvant therapy take before surgery?
The therapy itself may last 5–6 weeks, followed by a 6–8 week waiting period before surgery to allow optimal tumor response and recovery.
How successful is neoadjuvant therapy in shrinking tumors?
Many patients experience significant tumor shrinkage, making surgery easier and more precise. In some cases, the tumor disappears entirely on scans, though surgery is still often recommended.
What are the common side effects of this therapy?
Side effects can include fatigue, diarrhea, skin irritation at the radiation site, and mild nausea. Most side effects are manageable with supportive care.
Does neoadjuvant therapy improve survival rates?
Yes. Multiple studies have shown improved local control, reduced recurrence, and better overall survival when neoadjuvant therapy is used appropriately.
References:
https://my.clevelandclinic.org/health/treatments/neoadjuvant-therapy
https://www.sciencedirect.com/science/article/pii/S1040842823002846
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.

Low Anterior Resection Syndrome: Causes, Symptoms & Treatment
Low Anterior Resection Syndrome (LARS) is a common post-surgical condition observed in patients who undergo low anterior resection for rectal cancer treatment. It leads to bowel dysfunction, affecting the quality of life. LARS is a temporary problem that occurs as we save the anal sphincter and avoid permeant stoma.
According to Dr. Sandeep Nayak, a leading surgical oncologist in India, “LARS is a prevalent but manageable condition. With appropriate care, patients can regain bowel control and live comfortably. Timely symptom detection and effective management are crucial for this post-operative issue.”
With long-standing experience in surgical oncology, Dr. Nayak is an expert in complex colorectal cancer surgeries and post-surgery rehabilitation. With his team, he ensures patients receive individualized treatment protocols to deal with LARS effectively. Dr. Nayak and his team are well-known for their expertise in minimally invasive surgery and advanced cancer treatment in Bangalore, allowing quicker recovery with fewer complications.
What is Low Anterior Resection Syndrome (LARS)?
LARS is a group of symptoms occurring after low anterior resection (LAR). LAR is a surgical procedure designed to remove a portion of the affected rectum without removing the anal sphincter. LAR surgery is typically performed on patients with rectal cancer to maintain bowel continuity avoiding a permanent bag for stool collection, but can lead to bowel function abnormalities.
The rectum plays a vital role in controlling and storing stools.
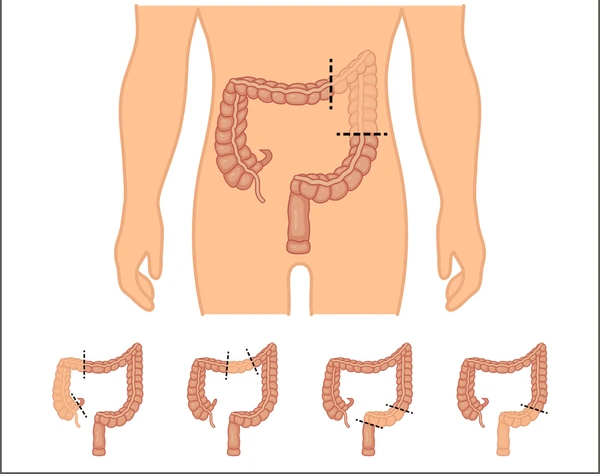
When a portion of the rectum is excised and modified, the body needs time to adapt, and the associated symptoms may persist for months to years. Adequate treatment and management of LARS can significantly improve the patient’s quality of life.
Do you have unexpected bowel changes after surgery? We will discuss the most frequent symptoms of LARS and how they impact daily living.
Symptoms of Low Anterior Resection Syndrome
Patients with LARS may experience:
- Frequent Bowel Movements– Needing to use the restroom multiple times daily.
- Fecal Incontinence– Some Loss of bowel control, with leakage at times, even when passing gas. This improves quickly after surgery.
- Bowel Urgency– Sudden, strong urge to defecate with little warning.
- Incomplete Evacuation– A sensation of not fully emptying the bowels.
- Constipation & Clustering – Alternating between hard stools and multiple small bowel movements in a short period.
- Gas and Bloating– Increased discomfort due to excess gas buildup.
- Unpredictable Bowel Habits– Irregular stool frequency and consistency, making daily life cumbersome.
- Nocturnal Bowel Movements– Bowel urges experienced at night, resulting in disturbed sleep.
“Most symptoms occur immediately after surgery. However, within one and a half to two years, most patients experience significant improvement and return to normal,” mentions Dr. Sandeep Nayak.
The severity of LARS symptoms is graded on a scoring system, which helps guide dietary modifications and other management strategies based on individual needs.
Identifying symptoms early can help control LARS better. Speak with a specialist for a personalized evaluation.
Managing Symptoms
The following strategies can help manage LARS:
- Dietary Adjustments
- Increase fiber intake gradually to regulate bowel movements.
- Avoid foods that trigger diarrhea, such as caffeine, dairy, and spicy foods.
- Stay hydrated to ease constipation and promote regularity.

- Pelvic Floor Exercises
- Pelvic muscle strengthening by some exercises can enhance bowel control.
- Kegel exercises tighten sphincter function and reduce incontinence.

- Toilet Routine
- Develop a regular bowel movement routine to promote regularity.
- Sit on the toilet and place a footstool to achieve an even better position for bowel emptying.
- Stress Management & Mental Well-being
- Reduce anxiety through meditation, breathing exercises, and counseling.
- Join support groups to connect with others experiencing similar challenges.

- Monitor Food Triggers
- Maintain a food diary to identify and exclude foods that trigger symptoms.
- Take small, frequent meals in order not to burden the digestive system.
Treatments for Low Anterior Resection Syndrome

Where lifestyle modifications are not sufficient, medical and sometimes surgical measures may be required:
- Medications– Loperamide anti-diarrheal medications delay bowel urgency, and fiber supplements thicken stools. Stool softeners may be used for constipation.
- Transanal Irrigation (TAI)– A method where the bowels are washed with water through a catheter to control the bowel movement and prevent incontinence.

- Dietary Counseling– A structured dietary plan created by specialists to balance fiber intake, avoid trigger foods and optimize digestion for better bowel control.
- Biofeedback Therapy– A technique that trains pelvic floor muscles to control bowel movement more effectively with the help of special sensors and therapist-guided exercises.

Conclusion
Low Anterior Resection Syndrome is a challenging condition, but with the right approach, symptoms can be managed effectively. From dietary changes to medical treatments, various ways exist to improve bowel function and enhance overall well-being. LARS will have to be managed in consultation with your treating doctors.
FAQs
What is anterior resection?
Anterior resection is a surgical procedure that removes a portion of the rectum affected by cancer while maintaining normal bowel function.
What is the best diet for low anterior resection syndrome?
A probiotic, fiber-rich, and well-hydrated diet can control bowel movements. Eliminate trigger foods such as milk, caffeine, and processed foods.
How long does low anterior resection syndrome last?
LARS symptoms last for years or months. Some patients recover slowly, but others need extended treatment.
What is the difference between anterior resection vs. low anterior resection?
Anterior resection involves the removal of upper segment of the rectum, whereas low anterior resection involves excising a lower portion of rectum while preserving the anal sphincter.
Reference links:
https://colorectalsurgery.wustl.edu/patient-care/low-anterior-resection-syndrome/
Disclaimer: This page is for informational purposes and not for promotional use.






