Natural Cancer Treatment – Safe or Unsafe?
Understanding Natural Products in Cancer Treatment

Dr. Nayak, a well-known surgical oncologist in India, explains:
“It may interest you that a group of medicines called taxanes are derived from tree bark. These alkaloids were refined through medical research to create chemotherapy drugs like Paclitaxel and Docetaxel. However, consuming raw tree bark without refinement means ingesting multiple unknown compounds. The problem lies in dosage control—too much can cause toxicity, and too little may be ineffective. Additionally, when taken alongside prescription medicines, natural products can dangerously amplify toxicity.”
While some natural compounds have led to medical breakthroughs, not all plant-based substances are safe or effective. Misusing them could lead to severe side effects, organ damage, or even interference with standard cancer treatments.
Still, many people believe that natural remedies are completely safe. Is this true?
Common Myths About Natural Remedies in Cancer Treatment

Many assume that because a remedy is “natural,” it must be safe. However, natural does not always mean harmless. Certain plant-based compounds can be toxic, causing liver damage, heart problems, or severe allergic reactions.
Myth 2: Herbs and supplements can replace chemotherapy
Some believe that chemotherapy alternatives such as herbal teas or special diets can treat cancer without the need for medical intervention. However, no scientific evidence supports this claim. Avoiding proven cancer treatments can allow the disease to progress unchecked.
Myth 3: If it worked for someone else, it will work for me
Personal testimonials and word-of-mouth recommendations are often misleading. Cancer treatments must be tailored to an individual’s medical condition, type of cancer, and overall health. A remedy that works for one person may not be safe or effective for another.
Dr. Nayak emphasizes:
“If you ask me as a qualified doctor, it is unwise to consume natural products during cancer treatment. Simply consuming raw tree bark or extracts can introduce unpredictable toxicity and interfere with ongoing treatment. If medical options are still available, they should always be the first choice.”
Risks and Realities: What You Need to Know Unpredictable Dosage

Potential Drug Interactions
Natural products can interfere with chemotherapy, radiation therapy, and other cancer treatments. Some plant compounds may reduce the effectiveness of medical treatments, while others may dangerously increase toxicity levels.
False Sense of Security
Relying on natural remedies instead of proven treatments can delay life-saving medical care. Some patients turn to alternative therapies in the hope of avoiding side effects, only to find that their cancer has progressed to an advanced stage.
Dr. Nayak, a trusted oncologist in Bangalore, cautions:
“If you are undergoing treatment, adding unverified remedies can create serious complications. Cancer drugs are designed for precision, and any additional substances can disrupt their intended effect. Natural products should only be considered when all medical options have been exhausted—and even then, with caution.”
Conclusion

Dr. Nayak reminds us:
“Medical research has come a long way in the fight against cancer. While alternative therapies may offer comfort, they should never replace evidence-based treatments. The best approach is to work closely with your medical team, make informed decisions, and trust in advancements that have been scientifically tested. Hope should always be accompanied by wisdom and caution.”
FAQs
Can natural remedies completely cure cancer?
Are there any natural products that can safely complement cancer treatment?
What happens if I take tree bark extracts along with chemotherapy?
Why do some cancer patients believe in alternative medicine?
What should I do if I want to explore natural treatments?
Dr. Nayak concludes:
“While the allure of natural remedies is strong, they should never replace professional medical care. Many of these substances contain active compounds that interact with prescription drugs unpredictably. The biggest risk is that patients may unknowingly increase toxicity or weaken the effectiveness of their treatment. When it comes to cancer treatment, science-backed medicine remains the safest and most effective approach.”
Reference Links:
https://www.webmd.com/breast-cancer/taxanes-breast-cancer
https://www.mskcc.org/news/truth-behind-three-natural-cures
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.


 Positron Emission Tomography (PET) scan, often combined with a Computed Tomography (CT) scan, is an advanced imaging technique that detects abnormal metabolic activity in the organs of the body. Commonly it involves injecting a small amount of radioactive glucose (FDG), which cancer cells absorb at a higher rate than normal cells, making them visible on the scan. There are other radioactive traces that are specific for some cancers like PSMA for prostate cancer and Dota for Neuroendocrine tumors.
Positron Emission Tomography (PET) scan, often combined with a Computed Tomography (CT) scan, is an advanced imaging technique that detects abnormal metabolic activity in the organs of the body. Commonly it involves injecting a small amount of radioactive glucose (FDG), which cancer cells absorb at a higher rate than normal cells, making them visible on the scan. There are other radioactive traces that are specific for some cancers like PSMA for prostate cancer and Dota for Neuroendocrine tumors.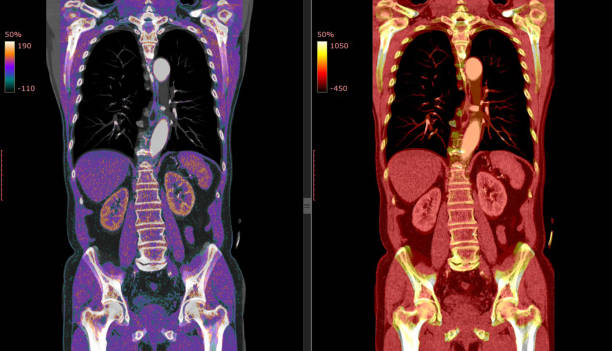
 1. It’s a Painless and Non-Invasive Procedure
1. It’s a Painless and Non-Invasive Procedure 1. Early and Accurate Detection
1. Early and Accurate Detection