10 Warning Signs of Liver Disease You Should Never Ignore
Liver disease encompasses a range of conditions that affect the liver’s ability to function correctly, leading to serious health problems if left untreated. Chronic liver disease, including conditions like cirrhosis, fatty liver, and hepatitis, can silently progress without noticeable symptoms in the early stages. However, when symptoms do arise, they can indicate liver damage that requires immediate attention.
Dr. Sandeep Nayak, a prominent surgical oncologist in India practising in Bangalore, explains:
“Liver disease often goes unnoticed in its early stages, but when symptoms appear, they should not be ignored. Timely intervention can prevent further liver damage and improve treatment outcomes.”
Dr. Nayak is renowned for offering cutting-edge, minimally invasive solutions for liver disease and liver cancer treatment at MACS Clinic in Bangalore. With years of expertise, he provides comprehensive diagnostic and therapeutic options, ensuring patients receive the highest standard of care for liver-related conditions.
In this blog, we will explore the 10 warning signs of liver disease that you should never ignore, helping you recognize when it’s time to seek medical advice.
What Is Liver Disease?
Liver disease refers to any condition that impairs the liver’s ability to function correctly. The liver is responsible for vital processes, including detoxifying harmful substances, producing bile for digestion, storing nutrients, and regulating various hormones. When the liver is damaged by conditions such as fatty liver disease, hepatitis, cirrhosis, or liver cancer, its ability to perform these functions is compromised, leading to severe health complications.
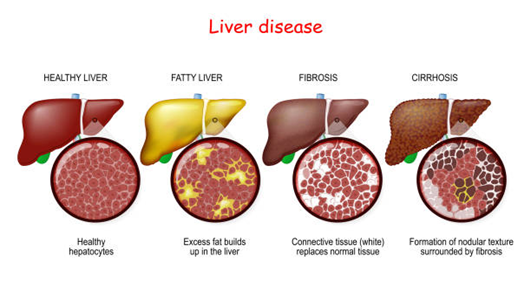
Is liver disease treatable, and can it be cured? Let’s explore this critical question.
Can Liver Disease Be Cured?
Whether liver disease can be cured depends on the type and stage of the condition. For conditions like non-alcoholic fatty liver disease (NAFLD) or hepatitis, lifestyle changes, medications, and regular monitoring can help manage the disease effectively. However, in cases of advanced liver disease, such as cirrhosis or liver cancer, a cure may not be possible, but treatments can slow progression and alleviate symptoms.
“In certain cases, a liver transplant may be necessary, particularly in patients with end-stage liver failure. Timely intervention and early diagnosis play a significant role in improving outcomes and preventing irreversible damage,” states Dr. Sandeep Nayak, a leading cancer specialist in India.
Why is early detection so important when it comes to liver disease? Let’s discuss.
Why Early Detection Matters
Early detection of liver disease is crucial because many liver conditions do not show symptoms until significant damage has occurred. In the early stages, the liver has a remarkable ability to regenerate, making it more responsive to treatment. Identifying liver disease early can prevent progression to more severe stages, reduce the need for invasive treatments, and improve the overall prognosis.
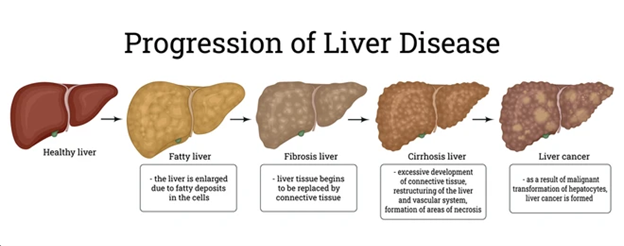
For example, detecting hepatitis or fatty liver disease early allows for lifestyle modifications and medications that can reverse liver damage. However, once cirrhosis or liver cancer develops, the treatment options become more limited, and the chances of a full recovery decrease.
What genes are associated with hereditary colorectal cancer, and how do they contribute to cancer risk? Let’s explore the key genes involved.
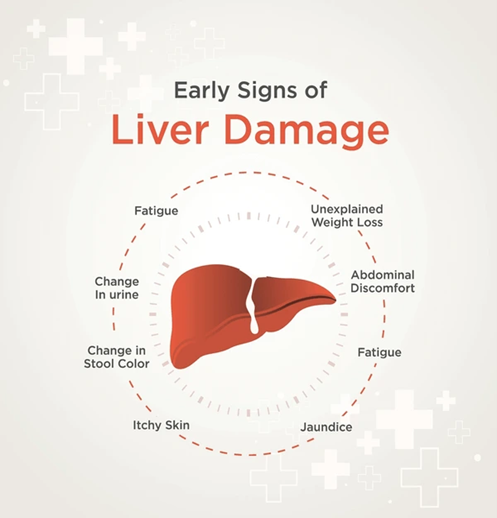
10 Common Warning Signs to Watch For
Specific gene mutations can make an individual susceptible to developing this cancer by disrupting the body’s ability to repair damaged DNA or regulate cell growth. To start with, some of the significant genes linked to hereditary forms of CRC include:
Jaundice
Fatigue
Feeling unusually tired or weak can be a sign that the liver is struggling to detoxify your body.
Abdominal pain and swelling
Pain in the upper right abdomen or swelling from fluid retention (ascites) can indicate liver inflammation or cirrhosis.
Loss of appetite
A sudden loss of appetite or unexplained weight loss can be a sign of liver dysfunction.
Nausea and vomiting
Persistent nausea or vomiting may be a symptom of liver disease, especially if paired with other warning signs.
Itchy skin
Persistent itching, particularly on the hands and feet, can be caused by bile buildup in the bloodstream, often due to liver problems.
Dark urine
Dark urine can indicate that your liver is not filtering toxins properly, leading to an accumulation of bilirubin.
Pale stools
Light-colored or clay-colored stools may suggest a problem with bile production, indicating liver disease.
Easy bruising or bleeding:
Confusion or disorientation:
Known as hepatic encephalopathy, confusion or memory issues can occur when the liver can no longer remove toxins from the bloodstream.
When should you seek expert advice for potential liver disease? Let’s break it down.
When to Seek Medical Help

If you notice any of the warning signs of liver disease mentioned above, it’s essential to seek medical help as soon as possible. If you have a family history of liver disease or are at high risk due to factors such as heavy alcohol consumption, obesity, or viral infections like hepatitis, early screening is recommended even if you don’t experience symptoms.
Dr. Sandeep Nayak, a distinguished surgical oncologist in Bangalore, advises, “Do not ignore persistent symptoms such as jaundice, unexplained fatigue, or abdominal pain, as they may be early indicators of liver dysfunction. Seeking help early can lead to better management of the disease and potentially prevent more severe outcomes like cirrhosis or liver cancer.”
How is liver disease diagnosed, and what tests are involved? Let’s take a look.
How Liver Disease Is Diagnosed
Liver disease is diagnosed through a combination of medical history, physical exams, and diagnostic tests. Some common diagnostic tools include:
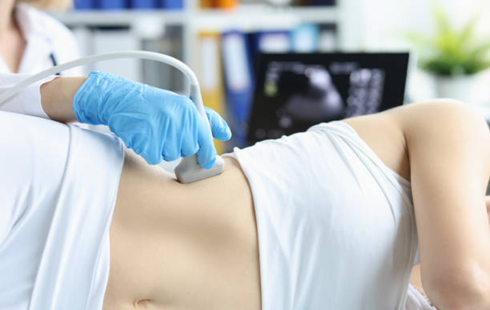
Ultrasound
An imaging test that provides a clear picture of the liver and can help detect abnormalities, such as tumors or fatty liver.
Blood tests
Liver function tests (LFTs) measure the levels of enzymes and proteins in the blood to assess liver damage.
CT scan or MRI
These imaging techniques provide detailed images of the liver to identify structural problems or signs of liver cancer.
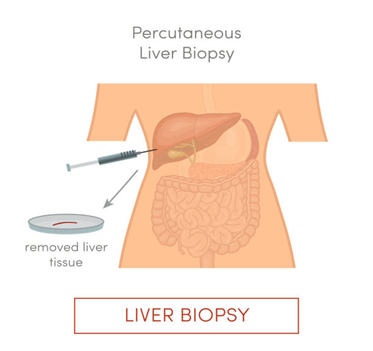
Liver biopsy
In some cases, a small liver tissue sample may be taken to assess the extent of damage or inflammation.
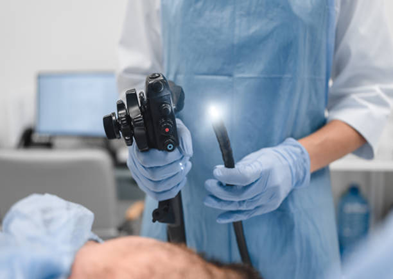
Endoscopy
If cirrhosis is suspected, an endoscopy may be done to check for varices or bleeding in the esophagus.
Conclusion
Liver disease can often develop silently, with few noticeable symptoms in its early stages. Recognizing the warning signs of liver disease early and seeking timely medical intervention can significantly improve the chances of successful treatment and prevent the progression of the disease. At MACS Clinic, Dr. Sandeep Nayak offers personalized care and cutting-edge diagnostic tools to identify and treat liver disease early, ensuring the best outcomes for his patients.
Frequently Asked Questions
1. What are the symptoms of a bad liver?
Symptoms of liver dysfunction include jaundice, fatigue, abdominal pain, loss of appetite, and swelling in the abdomen or legs.
2. How can I improve liver function?
Improving liver function involves maintaining a healthy diet, exercising regularly, avoiding alcohol, and getting vaccinated against hepatitis.
3. What is Stage 1 liver disease?
Stage 1 liver disease, such as fatty liver, often has no symptoms but is a precursor to more serious conditions like cirrhosis if left untreated.
4. What are the three early warning signs of liver disease?
The three early warning signs of liver disease are fatigue, abdominal discomfort, and jaundice (yellowing of the skin or eyes).
5. How do you cure liver disease?
While some forms of liver disease can be managed with lifestyle changes and medications, more severe cases may require a liver transplant or other advanced treatments.
Reference links:
https://my.clevelandclinic.org/health/diseases/17179-liver-disease
https://britishlivertrust.org.uk/information-and-support/liver-health-2/symptoms-of-liver-disease/
Disclaimer: The information shared in this content is for educational purposes and not for promotional use.