What Is a Permanent Stoma and How to Avoid It?
A permanent stoma is an opening made in the abdomen during surgery that redirects the bowel or urinary tract to an external bag on the body wall because the original exit route can’t be preserved, and whether you end up with one permanently comes down almost entirely to where your tumour sits, how advanced it is when it’s found and honestly how experienced the surgeon operating on you actually is with sphincter-preserving techniques.
According to Prof. Dr. Sandeep Nayak, Surgical Oncologist in India, “A permanent stoma is not inevitable for most rectal cancer patients. The right surgical technique and early diagnosis changes what’s possible on the table.”
What Is a Permanent Stoma and When Does It Happen?
These are the key things patients need to understand about permanent stomas:
- What it is: A surgically created opening in the abdomen wall where the bowel or urinary tract exits into an external bag because the normal pathway below has been removed or can’t function.
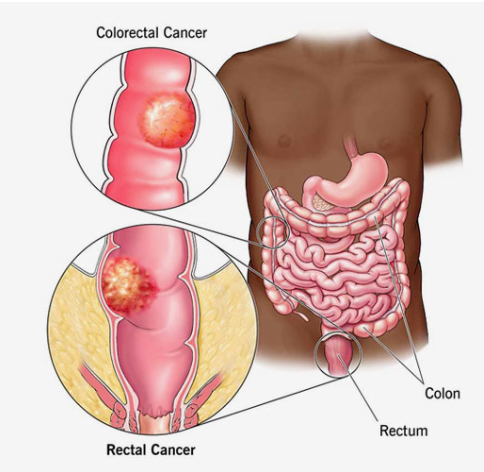
- When it’s unavoidable: Tumours sitting very low in the rectum close to or involving the sphincter muscle sometimes leave no way to reconnect the bowel and keep continence intact after removal.
- Temporary vs permanent: A temporary stoma gets reversed after the bowel heals from surgery, a permanent one stays because there’s nothing left below to reconnect to or the sphincter can’t function after what was done.
- Who decides: The tumour’s position on imaging and the surgeon’s honest assessment of whether sphincter preservation is safe and functional is what determines this, not a standard protocol applied to every case.
Most patients going into rectal cancer surgery don’t fully understand the difference between temporary and permanent until the conversation happens and by then some of them have already had the operation. Rectal cancer treatment at a specialist surgical oncology centre gives you the best realistic chance of avoiding a permanent stoma when the tumour location and stage actually allow for it.
How Can a Permanent Stoma Be Avoided?
These are the things that genuinely affect whether a permanent stoma can be avoided:
- Early diagnosis: A tumour found at stage one or two before it’s grown close to the sphincter is dramatically more likely to allow sphincter-preserving surgery than one that’s been growing quietly for eighteen months before anyone did anything about it.
- Neoadjuvant therapy: Chemoradiation before surgery shrinks locally advanced rectal tumours and a smaller tumour going into the operating room changes what the surgeon can achieve in terms of preserving the sphincter and avoiding permanent stoma.
- Surgical experience: Inter-sphincteric resection and ultra-low anterior resection are techniques that preserve the sphincter in cases where less experienced surgeons would tell the patient a permanent stoma is the only option and that gap in outcomes is real and documented.
- Robotic precision: Operating deep in the narrow pelvis close to the sphincter and nerve bundles is where robotic surgery genuinely earns its place because the magnified view and wristed instruments give the surgeon capabilities that hands in a tight space simply don’t have.
Whether sphincter preservation is realistic for your specific tumour is a conversation that needs your MRI, your staging and a surgeon who actually does high volume low rectal cancer surgery regularly. Colon cancer treatment covers the full colorectal surgical spectrum at specialist centres where avoiding unnecessary stomas is part of the surgical planning from the start.
Why Choose Dr. Sandeep Nayak for Cancer Treatment?
Dr. Sandeep Nayak has been doing rectal and colorectal cancer surgery for over 24 years and got deep into robotic and laparoscopic low rectal surgery at a point when most Indian centres weren’t attempting the sphincter-preserving techniques that make stoma avoidance possible in difficult cases. His MIND and RIA-MIND techniques were built specifically around operating in the narrow pelvis with the precision those situations demand. Dr. Nayak chairs Oncology Services across Karnataka and sees patients at MACS Clinic in Bangalore where the goal from the first consultation is preserving function wherever the tumour biology actually allows it.
Frequently Asked Questions
Can permanent stoma be avoided in rectal cancer?
Often yes, early diagnosis, neoadjuvant therapy and a surgeon experienced in sphincter-preserving techniques can avoid permanent stoma in many cases.
What is a permanent stoma?
An opening made in the abdomen wall that diverts the bowel to an external bag because the normal exit route below has been removed or can’t be preserved.
What is the difference between temporary and permanent stoma?
A temporary stoma gets reversed after bowel healing, a permanent one stays because there’s no viable bowel left below to reconnect to.
Does robotic surgery help avoid permanent stoma?
Yes, robotic precision in the narrow pelvis makes sphincter-preserving surgery possible in cases where open surgery would more likely result in permanent stoma.
Reference links:
- National Cancer Institute. Rectal Cancer Treatment. https://www.cancer.gov/types/colorectal/patient/rectal-treatment-pdq
- American Cancer Society. Surgery for Colorectal Cancer. https://www.cancer.org/cancer/types/colon-rectal-cancer/treating/surgery.html
- Disclaimer: The information shared in this content is for educational purposes and not for promotional use.