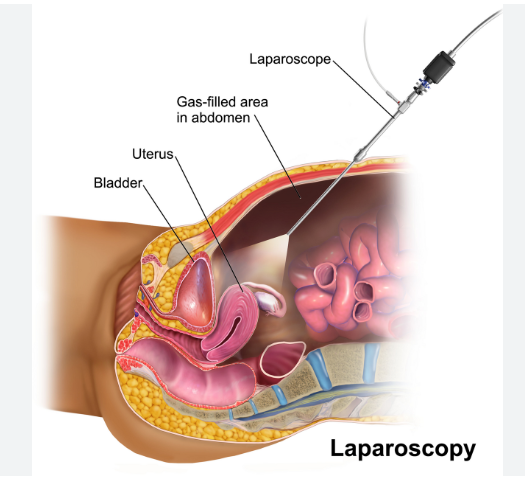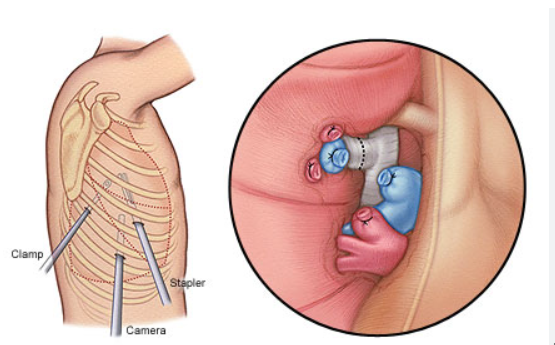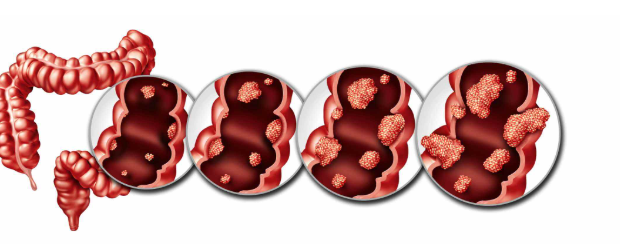
Survival Rate for Colon Cancer in India
Survival rates for colon cancer in India vary significantly depending on what stage the cancer gets caught at because someone diagnosed at stage one where the tumour is still sitting inside the colon wall has a genuinely good prognosis with five year survival above sixty to seventy percent at good surgical oncology centres while someone who comes in at stage four where cancer has already spread to the liver or lungs is looking at a completely different conversation and the honest truth is that the single biggest factor separating those two situations is almost always how early the person actually went to a doctor about symptoms they’d probably been noticing for a while.
According to Prof. Dr. Sandeep Nayak, Surgical Oncologist in India, “Colon cancer caught early is very treatable and survival outcomes in India at specialist centres have improved significantly but the problem is still that too many patients arrive late.”
What Do Survival Rate Numbers Actually Mean for Colon Cancer?
These are the things patients need to understand before reading survival statistics:
- Stage at diagnosis drives everything: Stage one and two colon cancer caught before it spreads beyond the colon wall carries five year survival rates that make complete recovery genuinely realistic, stage three and four are harder fights but not hopeless ones with the right surgical and oncology team.
- Five year survival is not the same as five years to live: A lot of patients hear five year survival rate and think it means something it doesn’t, it’s the percentage of patients alive five years after diagnosis not a sentence and many of those patients are alive well beyond that point.
- Indian data is getting better but early detection is still the gap: Survival outcomes at specialist surgical oncology centres in India have improved substantially over the last decade but the national average gets pulled down by late stage presentations that were preventable if symptoms had been acted on earlier.
- Where you get treated matters more than the statistics suggest: A five year survival rate is an average across every hospital, every surgeon and every stage and the outcomes at a specialist surgical oncology centre with high volume colorectal surgery experience look different from the average number you’ll find published.
Reading a survival statistic without understanding what went into it is one of the more anxiety-producing things a patient can do and it rarely tells you what you actually need to know about your specific situation. Colon cancer treatment at a specialist surgical oncology centre gives you outcomes that aren’t averaged across facilities that don’t do this at the same level.
What Factors Affect Colon Cancer Survival in India?
These are the real factors that determine how a colon cancer case plays out:
- How early the diagnosis actually happened: Stage one found during a routine check is a different disease trajectory than stage three found because symptoms got ignored for eighteen months and no statistic captures that individual difference.
- Whether the surgery got clear margins: The first operation is the most important one in colon cancer and a surgeon who gets complete resection with clear margins the first time gives the patient a head start that a re-operation or residual disease simply cannot undo afterward.
- Whether lymph nodes were involved: Node positive colon cancer needs chemotherapy after surgery and how well that’s managed, what drugs, what dose, what centre, all of it feeds into the five year outcome in ways the headline survival number doesn’t break down for you.
- The patient’s overall health and how well they tolerated treatment: Age, existing conditions, nutritional status, how the body handled chemotherapy if it was needed, these aren’t dramatic factors but they add up over five years in ways that change individual outcomes meaningfully.
Your survival outlook is a conversation between your specific tumour, your surgical team and your own biology and no published statistic covers that combination. This is worth reading to understand how surgical approach affects colon cancer outcomes in India.
Why Choose Dr. Sandeep Nayak for Cancer Treatment?
Dr. Sandeep Nayak has been doing colon cancer surgery for over 24 years and has been operating laparoscopically and robotically on colorectal cancers since before most Indian centres were taking minimally invasive oncology seriously as a discipline. Getting clear margins on a colon cancer resection the first time is exactly the kind of outcome his MIND and RIA-MIND techniques were built around delivering in difficult anatomical situations. Dr. Nayak chairs Oncology Services across Karnataka and sees patients at MACS Clinic in Bangalore where your colon cancer gets treated as the specific case it is rather than averaged into a protocol.
Frequently Asked Questions
What is the survival rate for colon cancer in India?
Stage one and two colon cancer has five year survival above sixty to seventy percent at specialist centres, stage four is significantly lower but still treated actively.
Does stage affect colon cancer survival rate in India?
Yes, stage at diagnosis is the single biggest factor and early stage colon cancer caught before spread has a genuinely good prognosis with the right treatment.
Is colon cancer curable in India?
Early stage colon cancer is very often curable with surgery and the outcomes at specialist surgical oncology centres in India have improved significantly over the last decade.
What improves colon cancer survival outcomes?
Early diagnosis, surgery with clear margins, appropriate chemotherapy where needed and treatment at a high volume specialist surgical oncology centre all meaningfully improve outcomes.
Reference links:
- National Cancer Institute. Colon Cancer Treatment. https://www.cancer.gov/types/colorectal/patient/colon-treatment-pdq
- American Cancer Society. Survival Rates for Colorectal Cancer. https://www.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/survival-rates.html
- Disclaimer: The information shared in this content is for educational purposes and not for promotional use.