In oncology, early detection and intervention play a vital role in saving lives. One area that requires special attention is the identification and management of precancerous lesions in the oral cavity. These lesions, also known as Oral Potentially Malignant Disorders (OPMD), are a significant concern as they can potentially progress into oral cancer if left untreated.

Oral cancer is a severe condition that affects millions of individuals worldwide. It often develops from precancerous lesions or potentially malignant disorders (OPMDs) in the oral cavity. Recognizing and understanding the precancerous oral cancer stages is crucial for early detection and effective treatment.
When it comes to treating oral cancer, having a trusted and experienced healthcare professional by your side is essential. Dr. Sandeep Nayak is a highly experienced surgical oncologist in India.
With over 15 years of expertise in the field, Dr. Nayak specializes in treating various forms of cancer, including oral cancer. His dedication to patient care and comprehensive approach makes him one of the best oncologists in India.
Dr. Sandeep Nayak’s expertise in the field of oncology has earned him the reputation of the finest cancer specialist, particularly for oral cancer treatment in Bangalore.
In this article, we will explore precancerous oral cancer, its causes, stages, treatment options, and prevention strategies.
First, let’s have an,
Overview of Precancerous Oral Cancer
Precancerous oral cancer, also known as oral potentially malignant disorders (OPMD), refers to the presence of abnormal tissue that can develop into cancer if left untreated.
When identified early, these lesions can be effectively managed, preventing the progression into malignancy. Understanding the different stages of precancerous oral cancer is essential to determine appropriate oral cancer treatment strategies.
Let’s know,
Why is it called Oral Potentially Malignant Disorder (OPMD)?
Oral Potentially Malignant Disorders (OPMDs) are a group of conditions characterized by abnormal changes in the oral tissues that have the potential to develop into oral cancer if left untreated. These disorders are precursors or warning signs of oral cancer and require careful monitoring and management.
OPMDs encompass various clinical presentations, including white or red patches, oral submucous fibrosis, and other potentially malignant lesions. Although not all OPMDs will progress to cancer, it is crucial to identify and monitor them closely to prevent further complications.
Causes and Location of Oral Precancerous Lesions

The exact cause of premalignant lesions of the oral cavity is not fully understood. However, certain risk factors increase the likelihood of developing these lesions; they may include:
- Tobacco use (smoking or chewing)
- Excessive alcohol consumption
- Betel nut chewing
- Chronic irritation from ill-fitting dentures or sharp teeth
- Poor oral hygiene
- Prolonged exposure to sunlight (lip cancer)
- Certain viral infections, such as human papillomavirus (HPV).
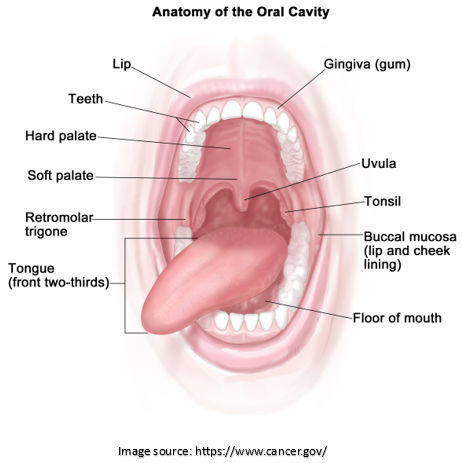
Precancerous lesions can appear in various parts of the oral cavity, including the tongue, floor of the mouth, lips, gums, throat and inner lining of the cheeks. Regular dental check-ups are crucial in identifying these lesions at an early stage.
Now, let’s discuss,
Precancerous Oral Cancer Stages
Precancerous oral cancer can be categorized into different stages based on the severity and progression of the lesions. The stages range from 1 to 4, with stage 4 being the most advanced.
The classification helps determine the appropriate treatment plan and prognosis for the patient. Timely diagnosis and intervention can prevent the advancement of these stages and reduce the risk of developing oral cancer.
Stage 1: Mild dysplasia (Abnormal cell growth)
- In this stage, the abnormal changes in the cells are mild and confined to the superficial layers of the oral mucosa. The risk of malignant transformation at this stage is relatively low.
- At this stage, the precancerous lesions are localized and have not invaded deeper tissues. Early detection and treatment offer the best chances of successful management.
Stage 2: Moderate dysplasia
- Lesions in this stage exhibit more pronounced cellular abnormalities involving a larger portion of the epithelial tissue. The risk of progression to oral cancer increases compared to mild dysplasia.
- The precancerous lesions have progressed slightly, involving a larger area within the oral cavity without invading deeper tissues.
Stage 3: Severe dysplasia
- In severe dysplasia, there is a high degree of cellular abnormalities throughout the epithelial layers. The risk of malignant transformation is significantly elevated, necessitating prompt intervention.
- In this stage, the precancerous lesions have further expanded and may have invaded nearby tissues. Lymph nodes may also be affected.
Stage 4: Carcinoma in situ (severe dysplasia with the potential to invade nearby tissues)
- At this stage, the precancerous lesion displays full-thickness dysplasia, resembling invasive cancer. Carcinoma in situ is considered the final stage before the lesion progresses into oral cancer.
- It is the most advanced stage, where the precancerous lesions have extensively invaded surrounding tissues and potentially spread to distant sites in the body.
Treatment for Precancerous Oral Lesions
The treatment for precancerous oral lesions depends on the stage, location, severity, and individual patient factors. Dr. Sandeep Nayak, one of the leading surgical oncologist in India, emphasizes the importance of personalized treatment plans tailored to each patient.
The treatment options may include surgical removal of the lesions, laser therapy, radiation therapy, chemotherapy, and targeted therapy.
Surgical intervention is often the primary treatment approach for precancerous lesions of the oral cavity. Surgery aims to remove the precancerous tissue or lesions to prevent the progression of invasive cancer.
The specific surgical technique employed depends on various factors, including the stage and location of the precancerous lesion. Here are some common surgical treatment options for premalignant lesions of the oral cavity:
1. Excisional Biopsy:
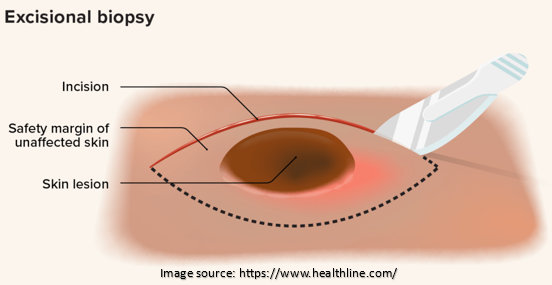
This procedure involves surgically removing the entire lesion or abnormal tissue. Often, surgeons perform this procedure when the precancerous stage is localized and easily accessible. The excised tissue is then sent for further examination to confirm the diagnosis and determine the extent of the lesion.
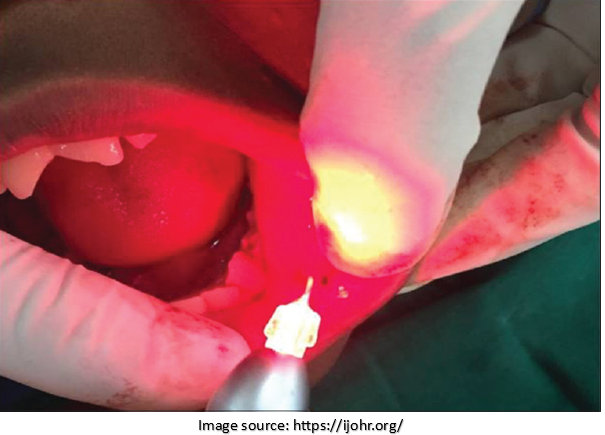
2. Laser Surgery:
Laser technology can precisely target and remove precancerous tissue. It offers the advantage of minimal bleeding, reduced trauma to surrounding healthy tissue, and faster recovery. Usually, surgeons perform laser surgery for small lesions or in areas where preservation of function and cosmetic appearance is crucial.
3. Cryosurgery:
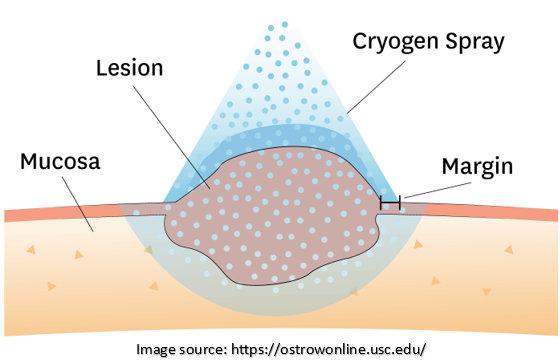
It involves freezing and destroying the precancerous tissue using extremely cold temperatures. This technique effectively treats superficial lesions and offers advantages such as minimal scarring, reduced pain, and a shorter recovery period.
4. Mohs Surgery:
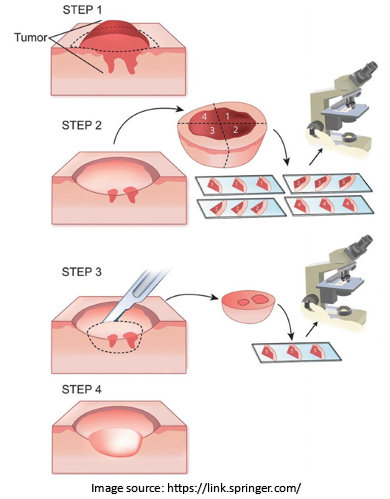
Mohs micrographic surgery is a precise technique that involves removing thin layers of tissue and examining them under a microscope in real-time. This process is repeated until no abnormal cells remain. Often, surgeons perform Mohs surgery for more extensive or recurrent precancerous lesions, offering a higher cure rate and preserving healthy tissue.
5. Electrosurgery:
This surgical procedure uses an electric current to remove or destroy precancerous tissue. Usually, doctors perform electrosurgery with other surgical techniques or to treat minor or superficial lesions.
6. Medications:
Oncologists may prescribe certain medications to control the progression of OPMDs and reduce the risk of developing oral cancer.
Prevention of Precancerous Oral Lesions
Preventing precancerous lesions of the oral cavity and reducing the risk of developing oral cancer is essential.
Here are some preventive measures to consider:
1. Quit tobacco use in any form.
2. Limit alcohol consumption.
3. Practice good oral hygiene, including regular brushing and flossing.
4. Eat a healthy diet rich in fruits and vegetables.
5. Protect lips from excessive sun exposure with lip balm or sunscreen.
6. Get vaccinated against human papillomavirus (HPV) as recommended.
Raising awareness about precancerous oral cancer stages, their causes, treatment options, and prevention measures is crucial in promoting early detection and improving patient outcomes.
By collaborating with experienced professionals like Dr. Sandeep Nayak, patients can access the expertise necessary for accurate diagnosis, personalized treatment plans, and comprehensive care. Remember, prevention and early intervention are key to maintaining oral health and reducing the burden of oral cancer.
Frequently Asked Questions
Q1. Is oral cancer serious?
A. Yes, oral cancer is a serious condition. If not detected and treated early, it can be life-threatening. It can spread to other body parts and significantly impact a person’s quality of life. Regular dental check-ups and self-examinations can aid in early detection and better treatment outcomes.
Q2. How do you treat oral precancerous lesions?
A. The treatment for pre-cancerous lesions of the oral cavity depends on the stage and location of the lesions. It may involve monitoring the condition closely, surgical removal of the lesions, laser therapy, topical medications, cryotherapy, or photodynamic therapy.
The treatment aims to prevent the progression of oral cancer and may require a multidisciplinary approach involving dentists, oral surgeons, and oncologists.
Q3: How often should I have oral cancer screenings?
A: Regular oral cancer screenings are essential, especially if you have risk factors such as tobacco or alcohol use. It is recommended to have screenings at least once a year during routine dental check-ups. Your dentist can determine the appropriate frequency based on your risk factors.
Q4: What are the risk factors for oral precancerous lesions?
A. Risk factors for precancerous lesions include tobacco and alcohol use, betel nut chewing, poor oral hygiene, human papillomavirus (HPV) infection, and genetic predisposition.
Q5. Are all precancerous oral lesions indicative of oral cancer?
A. No, not all precancerous oral lesions progress to oral cancer. However, one should take these lesions seriously and examine them with an expert healthcare professional.
Oncologists can assess the risk of malignant transformation through proper diagnosis and monitoring and implement appropriate treatment or management plans.


