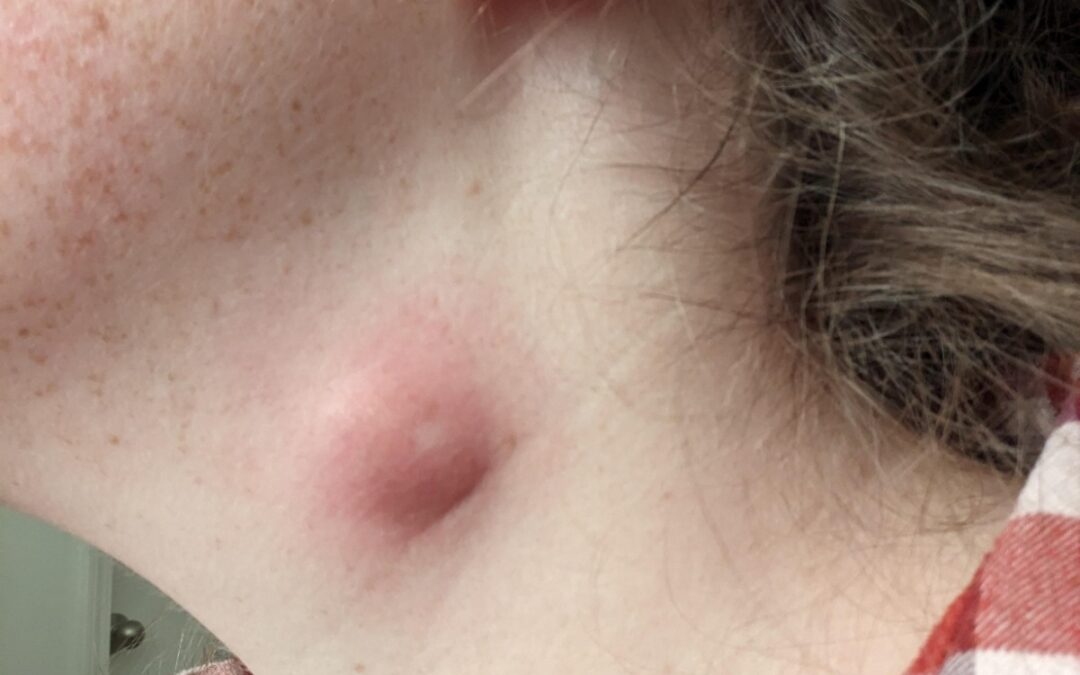
Why Won’t My Neck Lump Go After Antibiotics?
A neck lump that hasn’t resolved after a full course of antibiotics is no longer behaving like a simple infection, and needs specialist evaluation. The most common reasons are that the lump was never infectious to begin with, the cause is viral or atypical bacterial, it’s a benign cyst or thyroid nodule, or it’s a head and neck cancer that’s been mistaken for an infected lymph node. Standard ENT teaching is clear, if a neck lump persists beyond one antibiotic course, see a head and neck specialist within two weeks.
According to Prof. Dr. Sandeep Nayak, Surgical Oncologist in India, “A neck lump that won’t go after antibiotics is one of the most important patterns in head and neck oncology, because patients keep cycling through GPs for second and third antibiotic courses when the lump itself was never infection. That delay is what turns curable cancers into difficult ones.”
That stubborn lump deserves a proper answer, not another round of antibiotics.
Why Doesn't It Settle With Antibiotics?
The lump may simply not be the kind of problem antibiotics can fix.
- Not infection: The lump may have been a benign cyst, lipoma, thyroid nodule or reactive lymph node from the start, none of which respond to antibiotics in any way.
- Viral cause: Viral infections like glandular fever, mono or post viral lymph nodes cause swelling that antibiotics simply don’t touch, and need time or specific viral treatment.
- Atypical bug: TB lymph nodes, atypical mycobacteria or fungal infections need specific long course treatment, not the general antibiotic given for sore throat or skin infection.
- Something serious: A persistent lump can be head and neck cancer or lymphoma, where antibiotics have no effect and continuing them just delays the actual diagnosis.
So the lump not settling tells you the cause was never bacterial. For patients whose treatment involves surgery, robotic cancer surgery offers precise, recovery focused treatment as part of a complete plan for head and neck cancers.
What Should Happen Next?
A clear next step replaces another antibiotic course with real answers.
- See specialist: Book a head and neck surgical oncologist or ENT specialist within two weeks, not another GP. The right test gets ordered faster this way.
- Get imaging: An ultrasound of the neck is usually the first scan, often the same day, and tells you whether the lump is solid, cystic, glandular or suspicious.
- Biopsy ready: A small needle biopsy of the lump gives a clear answer, often within a few days, and is far less invasive than people fear.
- Note red flags: Track any weight loss, night sweats, voice change, mouth sores, ear pain or persistent swallowing trouble and share them all at the consultation.
So action replaces antibiotics when the pattern doesn’t fit infection. The same urgency applies to any persistent symptom in cancer care, our blog on biopsy delay explains why short waits matter more than patients realise.
Why Choose Dr. Sandeep Nayak for Your Breast Cancer Care?
Dr. Sandeep Nayak brings 24 years of surgical oncology experience, DNB qualifications in Surgical Oncology and General Surgery and a fellowship in Laparoscopic and Robotic Onco Surgery to the care of patients across head and neck cancers. He evaluates persistent neck lumps with ultrasound and biopsy in the first consultation rather than sending patients back for more antibiotics, so cancers in this group get caught at their most treatable stage.
That refusal to keep cycling antibiotics on a non infection lump is what changes head and neck cancer outcomes. Every case at MACS Clinic goes through a full tumour board, where the diagnostic plan is set together. Call +91 8104310753 to book your consultation.
Frequently Asked Questions
Why isn't my neck lump going after antibiotics?
It may not be infection, needs specialist evaluation and imaging now.
How long after antibiotics should a lump settle?
Within two to three weeks, anything longer warrants specialist review.
Could it be cancer?
Possibly, persistent neck lumps need a head and neck specialist.
What tests are done next?
Ultrasound, biopsy and imaging like CT or MRI.
References:
- National Cancer Institute, Head and Neck Cancers. https://www.cancer.gov/
- World Health Organisation, Cancer. https://www.who.int/news-room/fact-sheets/detail/cancer





